Three healthcare workers on the front lines of the world’s disease epidemics have been recognised for their commitment and bravery.
The trio were recipients of the Reach awards at the Reaching the Last Mile forum at Louvre Abu Dhabi on Tuesday.
Rahane Lawal, Richard Kojan and Olivia Ngou worked to tackle polio, Ebola and malaria, respectively – among the debilitating diseases the forum was set up to tackle by raising funds for research.
Ms Lawal, from Nigeria, saw her stepfather shot in front of her and was held hostage by bandits until her family paid a ransom, while Dr Kojan built special containment units to allow medics to safely treat Ebola patients at the height of the outbreak in the Congo.
Here are their stories:
Rahane Lawal, Unsung Hero
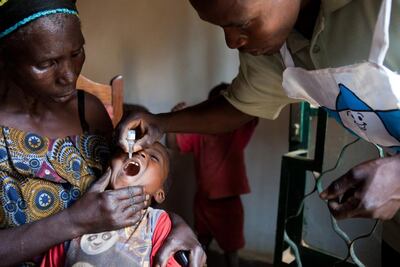
Few people have paid a higher price for their commitment to vaccinations than Rahane Lawal.
As a Unicef volunteer, she travels to communities in Nigeria, persuading parents to accept inoculations for their children and countering myths that once led to health workers routinely being turned away.
Last year, a gang of bandits broke into Ms Lawal’s home, demanding a large sum of money they wrongly believed she had been paid for her work.

She had a gun held to her head in front of her young daughter, and her father-in-law, who had encouraged her to join the Unicef programme, was shot dead.
Ms Lawal was held hostage for 11 days, until her family and community members raised enough money to satisfy her captors and secure her release.
In an interview with The National, she said she found the experience too upsetting to talk about, with her experience instead relayed by a translator who was familiar with her story.
But despite the trauma, she had continued with her work, moving to a new area in northern Nigeria and continuing to convince people of the benefits of vaccines.
“It has become my passion,” Ms Lawal, 51, who has been volunteering for five years, said. “I had seen kids that had become crippled from polio.
“We had issues of parents not accepting the polio vaccine. There were a lot of myths – people used to believe that once they gave children the vaccine the child would become infertile.
“That people were following them, offering the vaccine free when treatment for conditions like malaria was not free, made people suspicious.
“But I have 10 children and I used my children as an example, because all my 10 kids had their vaccinations. So I showed them ‘look how healthy my kids are’. That has been able to persuade them.”
Unicef and other charities use local community members to spread a pro-vaccine message, as they are more effective than outsiders, and people like Ms Lawal also enlist the help of trusted religious leaders to improve uptake rates.
She has helped achieve “record successes” in Nigeria, which has gone three years without a case of polio and is close to being declared free of the disease.
“Being recognised with the award has given me even more strength to go back and do more,” she said.
“But we still have so many communicable diseases, so we want the world to really support Nigeria to fight all these other diseases like malaria and typhoid which are still out there.
“We also need help in the fight for security, because we have not been able to go to certain communities because of the security situation. So the insecurity needs to be addressed.”
Dr Richard Kojan, Game-Changing Innovator
When Richard Kojan, a Congolese doctor, joined the fight against the first Ebola outbreaks in Western Africa between 2014 and 2016, he was left “frustrated” by the quality of care he was able to provide.
The highly infectious nature of the disease meant he had to wear cumbersome protective equipment and could not spend much time with his patients. For those affected, contact with friends or family was out of the question.
There was also a shortage of suitable facilities for treating Ebola patients, who, if they survive, spend an average of 16 days in isolation.

“I am an ICU doctor, so I like to spend time with my patients, give them care and support them,” Dr Kojan, 48, said. “It was not possible to give really good care for the patients. So I started to think and wanted to build some new tools.”
His answer was the Cube – an airtight, pressure and temperature-controlled chamber made of see-through, plastic walls. It allows doctors to treat patients through the walls, cutting the risk of exposure and contamination and also giving Ebola sufferers the opportunity to get emotional support from loved ones. Doctors can even deliver babies through the Cube, if patients are pregnant.
“With the Cube I can work with the patient, give food and provisions, put electrodes for monitoring – all the patient needs, I can give,” Dr Kojan said. “It makes a difference – it’s changed life for the patients and health workers. So I have come here to Abu Dhabi to share my tool, my experience.”

The invention has featured prominently in The Lancet, the prestigious medical journal. Each device costs €16,000 (Dh65,000), less than the cost of a traditional intensive care unit, and can be easily transported. It can also be used for patients with other illnesses, such as Rift Valley fever.
And while Dr Kojan is pleased with the progress made on tackling Ebola in a few short years, he wishes other conditions received the same attention.
“Today, Ebola is not an incurable disease,” he said. “Now, we have to continue to push with research. But, for me, it is not just about Ebola – there are many diseases in Africa and many patients die.
“We need the same mobilisation for measles, malaria, dengue. Eliminating Ebola would not be enough – we have to continue.
“We also have malnutrition. Many children die because they don’t have food, and we are starting to see the effects of climate change. So we need more and more support.”

He would like to see more action from the world’s politicians, he says, as well as more funding. He called for new research in the West, with the findings applied in Africa, as well as a greater use of technology so people in isolated parts of the continent can have access to the same standard of care as those in towns and cities.
Medical tests that could once only be carried out in clinics with expensive equipment, he points out, can now be performed using smartphones.
“To me, the situation is not acceptable,” he said. “We have to change. Today, there is no reason that only in the towns they can have a good standard of care, because the technology today makes such a difference. We have just to bring this technology to everyone.
“For me, it’s unacceptable to have low standards in the village, we have to stop this nonsense. And for me it is nonsense.”
Olivia Ngou, Rising Champion
When Olivia Ngou graduated from university in New York with a public health degree, she knew what she wanted to achieve.
While growing up in Cameroon she had malaria several times, including a serious case when she was a young girl.
So after working on combating the disease as a UN intern, she co-founded the Civil Society for Malaria Elimination, an NGO, in her home country. It brings together politicians, celebrities, charities, the media and others to focus on eliminating malaria.
The organisation, which she leads, has help persuade to Cameroon government to increase funding for fight malaria by 400 per cent.
“I realised it was possible to end the disease in this generation so I focused all of my work for the past 10 years on malaria advocacy,” Ms Ngou, 34, said.
One particular episode stands out in Ms Ngou’s mind – when she had a severe bout of malaria at age eight.
“Each person has a different reaction to that – for me it was hearing,” she said.
“I would hear your voice 10,000 times louder [than usual] and I would tell everyone ‘stop screaming, stop screaming’ and nobody was screaming.”
She recovered, because her parents were able to pay for treatment, and she knows she is one of the lucky ones.
“It was a bizarre experience and everyone has a different experience,” she said.
“Unfortunately some people have a cerebral malaria and the damage is awful, and some people are also crippled, so it depends on how your body would react.”
Among the celebrities she has enlisted to help raise awareness are Didier Drogba and Samuel Eto’o, the footballers, Lady Ponce and Youssou N’Dour, the singers, while Richard Bona, the Cameroonian bassist, helped create an anti-malaria anthem.
“It was actually easy to get them to help because every single celebrity that had lived in Africa had malaria or knows someone who had malaria,” she said.
“For example, Samuel Eto’o has said ‘if I didn’t have treatment I wouldn’t be here – I wouldn’t have become one of the greatest players in the world.”
She remains concerned, however, that malaria is not being taken as seriously as conditions such as Ebola and HIV, despite it being responsible for far more deaths.
“One of our biggest challenges is to actually make people understand the real danger of malaria because it is a disease that is so common – people have it so many times – that there is a need to reinforce the message around the danger,” she said. “It is the oldest and deadliest disease in human history.”
Despite progress in Cameroon, there are still between 2,000 and 3,000 documented deaths from malaria per year, and the true total is likely to be higher. Ms Ngou is also concerned about growing resistance to treatments to malaria in South East Asia, as mosquitoes evolve. If this is repeated in Africa, it could be the “worst public health problem that we have seen,” she said, and makes tackling malaria even more urgent.
But funding in some countries has “stalled”, she said, as issues like global warming and security challenges suck up cash and attention.
“We don’t have time [because of] this resistance issue,” she said. “We have to make sure that we can quickly invest. We know if you invest in malaria you will see the result quickly, like we saw in the last 15 years.
“Malaria has been here for so long, do people even believe [it is possible] to eradicate it? They have to believe it is possible.”