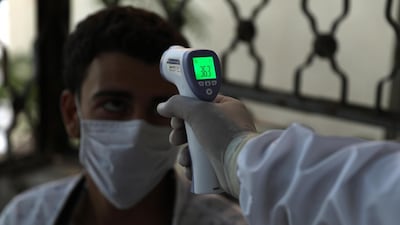
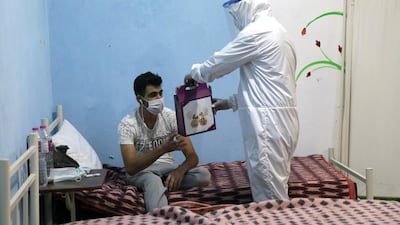
National Editorial: We cannot allow ourselves to tire in the fight against Covid-19
Cases of Covid-19 are on the rise again. In Europe, South Korea, Australia and elsewhere, countries that successfully controlled the virus are now seeing a spike in cases.
The UAE is among the many nations to once again consider localised lockdowns, with officials warning of a 'second wave' if the public does not act responsibly.
Yet like many other countries, the increase in cases here has not been matched by a surge in deaths. So is the virus becoming less deadly - or are we witnessing the calm before the storm of a second wave of Covid-19?
What do the statistics show?
Globally, the Covid-19 pandemic is still raging, with over 24 million cases resulting in over 800,000 deaths so far. Yet many countries who appeared to have successfully controlled the virus are now seeing renewed surges in Covid-19 cases.
Since the end of June, Spain and France have witnessed almost a ten-fold surge in new infections, now running at several thousand a day.
Even South Korea – widely regarded as a paragon of disease control - has seen a five-fold rise in infections this month, and on Tuesday closed schools in the capital, Seoul. Germany, Italy and the UK are also seeing case numbers rise, though far less dramatically.
In the UAE, the number of cases has crept up to several hundred a day. Active cases rose by 10 per cent in August.
Yet the surge in infections seen in many countries has not been mirrored by rising numbers of deaths, which have largely continued to fall or remain static.
Is the virus getting less lethal?
This is the most obvious explanation. It also fits in with the theory that pandemic viruses tend to mutate into less deadly forms, as they have a better chance of being transmitted if they don’t kill their human hosts.
However studies of Sars-CoV-2 - the scientific name for the coronavirus, which causes Covid-19 - suggest it has a relatively slow mutation rate.
As such, a substantial decrease in its lethality is unlikely to have taken place over recent months.
Are we just getting better at treating the disease?
Greater knowledge and better treatments – such as the use of dexamethasone – have cut death-rates among the seriously ill. While in March almost 60 per cent of Covid-19 patients in intensive care units died, this figure dropped to around 40 per cent by May and is still falling.
However, this can’t explain why the surge in infections has led to virtually unchanged death rates.
Are we simply seeing more cases by testing more people?
This is widely seen as a key part of the explanation. In the early days of the pandemic, many countries were forced to limit tests to people already showing signs of Covid-19 and thus more likely to die from it.
Now the greater availability of testing is leading to positive results from people with mild infections who are much less likely to die.
This weakens the link between number of cases and numbers of deaths. It’s even possible that the actual number of infections has changed little over recent months, and the surge is largely due to detecting cases that were already there.
Isn’t it mainly young people who are driving up the cases?
With testing now more widely available, it is also covering more of the population – especially younger age-groups, who are known to be at substantially lower risk of dying from Covid-19.
A recent international study suggests that while the mortality rate among those over-80s who become infected is around 1 in 10, this plunges to around 1 in 100 for those between 60 and 69, and is close to zero for those under 40.
This has prompted fears that re-introducing lockdowns in response to the surge in cases will cause major economic damage in return for little health benefit, as most people of working age are at negligible risk.
So should restrictions apply only to older adults and the vulnerable?
Some epidemiologists argue for a focused approach to dealing with the surge in cases, based on so-called "stratified" restrictions based on age and health status. Some studies suggest limiting restrictions on around 15 per cent of the population would strike the right balance between protecting the vulnerable and health services while not threatening economic recovery.
There is tentative evidence that people in high-risk categories may have already adopted this strategy voluntarily.
An analysis by the Financial Times of UK statistics show that while new infection rates have surged among younger people since early June, they have plunged among men over 70 and women over 50. This may partly be due to those in these age-groups deliberately taking action to avoid infection.
Should we just ignore the surge?
Not at all. While the surge may be taking place primarily among younger people with very little chance of dying, they remain capable of passing it on to older, more vulnerable people. This risk is likely to increase as more young people are compelled to move back in with their parents because of economic hardship.
Dying from Covid-19 is not the sole outcome of becoming infected, in any case: studies have found that many of those who appear to defeat the virus can still suffer debilitating long-term effects, including organ damage.
Robert Matthews is visiting professor of science at Aston University, Birmingham, UK