An Abu Dhabi resident has made a full recovery after suffering a rare type of stroke that initially presented as a severe headache and was not detected in early examinations.
Emirati Rashed Al Kaabi, 41, first experienced symptoms in January, shortly after finishing his evening prayer.
“It felt like something hit me hard on the head,” Mr Al Kaabi said. “It was a headache I had never felt in my life.”
At the time, he was preparing to celebrate his wedding anniversary with his wife, who was seven months pregnant. Despite the severity of the pain, Mr Al Kaabi initially tried to manage it at home.
“I tried to sleep it off. I took painkillers. I even tried to eat something, but I almost threw up,” he said. “I’m not someone who usually gets sick.”
About 13 hours after the pain began, he went to the emergency department. Doctors conducted neurological checks, including balance and vision tests, which appeared normal.
“They gave me strong painkillers and told me to observe myself and come back if it didn’t improve,” he said.
Increased problems
Over the following days, the headache persisted, but medication made it manageable enough for him to continue his routine.
“I went back to my normal life. I went to work, I drove, I attended training,” he said. “The pain was there, but I was controlling it with the medication.”
By the fourth day, the pain became unbearable.
“By Tuesday, it was too much. I couldn’t handle it any more,” the father of three said.
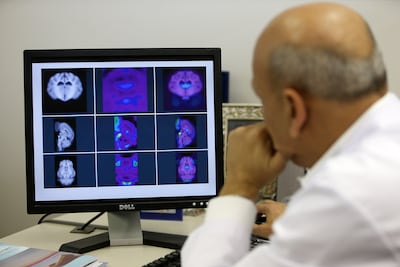
He went to the emergency department at Cleveland Clinic Abu Dhabi where doctors ordered a CT scan which revealed bleeding at the back of his brain.
“They asked my wife to sit down,” he said. “Then they told us there is bleeding.”
Further tests confirmed that Mr Al Kaabi had suffered a haemorrhagic stroke, caused by a dural arteriovenous fistula (DAVF), an abnormal connection between arteries and veins in the covering of the brain.
“Strokes are broadly divided into two types. Ischemic strokes are caused by blockages, and haemorrhagic strokes involve bleeding,” said Dr Mohamed Samy Elhammady, a staff physician in the Neurosurgery Department at Cleveland Clinic Abu Dhabi’s Neurological Institute.
“In this condition, arterial blood flows directly into veins under high pressure, and those veins are not designed to handle that pressure. That can lead to rupture and bleeding.”
The condition is rare, with an estimated incidence of 0.1 to 0.3 cases per 100,000 people annually, and may not cause symptoms until complications occur.
Mr Al Kaabi was admitted for treatment and underwent an angiogram to map the blood vessels in his brain.
“They explained everything, what was happening and what they were going to do,” he said.
Doctors first attempted two minimally invasive endovascular procedures, using a catheter to deliver a glue-like material to block the abnormal connection.
“The goal is to close the draining vein. Once that is closed, the fistula shuts down,” Dr Elhammady said.
Eight-hour long brain surgery
However, due to the complexity of the vessels, the procedures could not fully resolve the condition. Doctors then performed open brain surgery lasting more than eight hours, placing clips to close the abnormal connection.
“It was complicated because the vessels were very narrow,” Mr Al Kaabi said. “But they managed to fix everything.”
Mr Al Kaabi remained in hospital for more than two weeks. He has since returned to normal life with no lasting neurological effects.
“I don’t have any issues with my balance, my vision or my memory,” he said. “It’s as if nothing happened.”
In many cases, including Mr Al Kaabi’s, there is no clear cause.
“I asked why this happened to me,” he said. “They told me it could be something I was born with, or something that developed over time. There’s no specific reason.”
However, Dr Elhammady said some cases are associated with certain conditions.
“These fistulas can occur spontaneously,” he said. “But they are sometimes seen in patients with prior head trauma, previous brain surgery, or conditions that increase blood clotting.”
He added that clotting in the brain’s venous system may play a role in how these abnormal connections develop.
Some patients may experience warning signs such as persistent headaches, ringing in the ears or visual disturbances, while others remain asymptomatic until a haemorrhage occurs.
If untreated, the condition can be life-threatening.
“The risk of a second bleed is significant, particularly in the weeks following the first haemorrhage,” Dr Elhammady said.
Mr Al Kaabi said the experience has changed how he responds to symptoms.
“Don’t ignore anything,” he said. “We always think it’s just a headache or lack of sleep, but you have to listen to your body.”
He also highlighted the importance of support during recovery.
“It’s very important to have a strong support system,” he said. “It’s hard on you and it’s hard on your family.”



