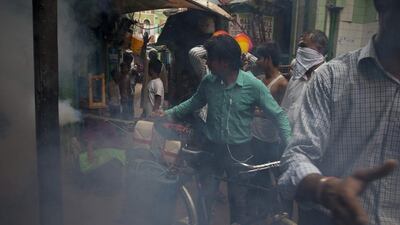NEW DELHI // At dusk, the foggers come out to spray their sticky-sweet clouds of diesel smoke and insecticide across the Indian capital. Mothers scold their children for wearing short sleeves. Posters glued to signposts warn about the perils of neighborhood puddles.
Such efforts to stop mosquitoes from spreading dengue fever in New Delhi have failed to keep the city from its biggest outbreak in almost two decades: more than 10,190 registered cases, including 32 deaths. Experts say it didn’t need to be this way, and blame health officials for being slow on both prevention work and medical response.
They say, for example, that the Delhi municipal government should have started much sooner and anticipated a longer-than-usual mosquito-breeding season months ago, when weather forecasters predicted this year’s monsoon would extend beyond September.
“If they clean up in time, if they have those anti-mosquito, anti-larval measures on time, they can contain dengue,” general physician Devendra Jain said in the small single room, crammed with patients, where he operates his private practice in south Delhi.
Some officials reject the idea that the high numbers are a result of neglect, and instead say they prove the city is simply conducting more tests. Some infections go unreported every year because some people with dengue fever don’t seek medical treatment, and others visit doctors who don’t report cases.
Health officials also note that while the number of cases this year has almost surpassed the 1996 high of 10,252, the death toll is far lower than the 423 who died from dengue 19 years ago. There are no statistics on dengue for years before 1996.
Three weeks into October, new cases were still being reported. The Holy Family Hospital alone said it was still detecting about 27 cases a day on average, down from a September peak of 75 cases a day.
Dengue leaves its victims exhausted and in great pain, though it is rarely fatal, claiming less than 1 percent of those infected. There is no cure; patients need rest and to be monitored and treated for symptoms, including high fever, dehydration, skin rash, exhaustion and a low blood platelet count.
“It is not rocket science,” said Manish Kakkar, a researcher at the Public Health Foundation of India, a research and consulting group. “We know what we have to do, but what happens in India is that the public health measures are not adequate both in terms of quantity and quality.”
The dengue outbreak has highlighted India’s striking health-care inequalities. It is home to a $4 billion medical tourism industry – offering everything from bargain tummy tucks to experimental stem-cell treatments – and to hundreds of millions of impoverished Indians who still have no access to trained doctors or basic medicine.
When two young boys died last month after their parents said they were denied treatment at private hospitals, India’s Health Minister warned the government would yank licenses from any hospitals who turned patients away.
State-run hospitals canceled doctors’ vacations, ordering them back to work. Delhi capped the cost of lab tests at 600 rupees ($10) and set up 55 “fever and dengue clinics” to handle the throngs of patients crowding into hospital foyers. Just one of those clinics, near Jamia Millia Islamia university on the southern outskirts of New Delhi, reported screening 800 patients a day.
Some doctors complain that many people seeking medical attention don’t need it, and blame the media for hyping the outbreak.
“Basically there is a panic and patients are very scared,” said Dr. Sonika Bali, the medical officer in charge at one government clinic, whose own 12-year-old daughter was among those infected. “We can’t have every patient come in and ask for a blood test. It is becoming very difficult to convince patients that their symptoms are not that of dengue.”
Some who truly have dengue, meanwhile, wait before seeking treatment, worsening their symptoms.
Noor Jehan had aches and pains for days before seeking help. By the time she finally visited the clinic, she had become so weak her husband had to pick her up from her housekeeping job and take her home in a wooden cart.
“My legs hurt,” the 40-year-old Jehan said. “I would get chills at night.”
Tejaswi Sharma, a 34-year-old software engineer, waited even longer for a diagnosis – until his body went into shock and his kidneys malfunctioned.
“When I first had a fever, I went to my doctor,” but he didn’t test for dengue and instead told Sharma he probably had the flu, he said. “My health deteriorated so fast that I started having breathing problems.” That’s when Sharma’s mother took him to Holy Family.
Argentine lawyer Laura Vassallo was struck with dengue during the first week of her six-month “dream trip” to India, and said her own country was much more proactive in fighting dengue. No water is left to stagnate, she explained. “They are very, very strict with the cleaning, and no throwing garbage on the streets.”
People who live outside the areas covered by the city’s anti-mosquito program try to ward off mosquitoes any way they can – including hiding under mosquito nets or generating plumes of smoke by burning egg crates, incense or whatever is at hand.
“Certainly this is a peak year for dengue,” said Babita Bisht, chief entomologist of the North Delhi Municipal Corporation. Her teams are working through weekends to visit all city neighborhoods, fumigating foliage to kill mosquitoes and spraying puddles to kill their larvae.
They also hold events to inform citizens of the risks, urging them to cover up in clothing and mosquito repellent. Newspapers, meanwhile, carry full-page discussions on which perfumes or house plants might keep mosquitoes at bay.
“Spraying outside in the open may not kill so many mosquitoes,” Bisht said, “but it makes the public aware.”
* Associated Press