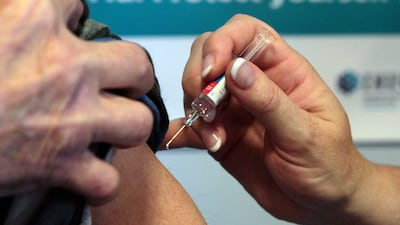
The coronavirus that emerged more than three and a half years ago continues to evolve, most notably with the recent emergence of the EG.5 variant.
EG.5 has become one of the most common forms of the virus in countries including China, South Korea, Japan and the United States.
Reports indicate that hospital admissions have increased in some countries in Asia where EG.5, also known as Eris, has become prevalent.
As The National reported this week, EG.5, which is a descendent of the fast-spreading Omicron variant, has now reached the Arabian Gulf region, having been detected in Kuwait.
Here we look at the significance of Eris and consider the continued need for vaccines to protect against Covid-19.
When did Eris emerge?
Eris was first detected in February and was named as a variant by the World Health Organisation (WHO) in July as case numbers increased in some countries.
Earlier this month, EG.5’s status was upgraded to variant of interest by the WHO amid concern that the variant may spread faster and be better able than previous variants of the virus to evade the protection provided by the immune system.
Gavi, the vaccines alliance, states that EG.5 is similar to XBB.1.5, which is another Omicron descendant. In the northern hemisphere last year, XBB.1.5 was the cause of many infections in winter.
"It does appear to be more infectious or to spread more readily," Paul Hunter, professor in medicine at the University of East Anglia in the UK, said of EG.5.
Eris has a change to the spike protein known as an escape mutation that makes it more capable of breaching existing immunity, whether from previous infection, vaccination or both.
"Because of that it’s increasing," Prof Hunter said. "It’s now about somewhere like 20 per cent to 30 per cent [of cases] across most countries. It’s probably going to become dominant and will drive up infections a bit."
How much of a concern is Eris?
While saying that Eris would probably increase the number of cases, Prof Hunter said that "there’s no evidence it causes more severe disease".
The mechanism that confers immunity to severe disease is different to that behind immunity to infection and for this reason, Prof Hunter said, Eris is not causing people to become more ill when compared with infection from other variants.
Ian Jones, professor of virology at the University of Reading, said that the increase in case numbers with Eris was typical of when a "new variant knocks out the old".
"Increased transmission does not equate to increased risk," he said. "What it will mean, however, is another wave of Covid at some level, which will be of concern to those generally vulnerable to respiratory infections."
WHO figures indicated that seven-day case numbers globally more than doubled in the space of a week in late July, increasing from 331,308 on July 24 to 672,959 on July 31.
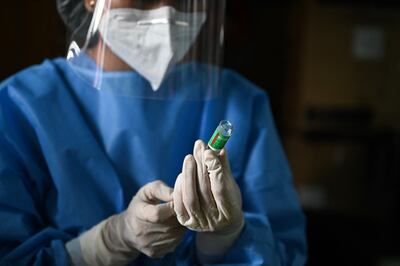
What is the vaccine situation like as Eris becomes more prominent?
Several of the major vaccine producers – Moderna, Pfizer-BioNTech and Novavax – are said to be readying new vaccines that are better tailored to provide immunity to the most common variants.
These follow the release last year of "bivalent" vaccines, which target the original coronavirus and the Omicron variant.
Possibly likely to be offered as soon as next month, according to the news agency Reuters, the new jabs have been developed with the XBB.1.5 variant in mind. Because EG.5 is very similar, it should find it harder to evade the immunity of these updated vaccines.
However, in some major countries, including the US, Covid-19 vaccine uptake has fallen as concern over Sars-CoV-2, the virus that causes Covid-19, has declined.
Indeed, Reuters reported forecasts from analysts that Pfizer and Moderna will have vaccine sales of $20 billion this year, down from $56 billion in 2022.
What do experts say about the need to get vaccinated against Covid-19?
John Oxford, emeritus professor of virology at the University of London, cautioned against emerging complacency over the risks posed by Covid-19, saying that "vaccination is the key".
"It’s at the centre of things with Covid. It still is," he said. "With flu you don’t stop vaccinating, you continue your vaccination. I would encourage everyone to continue the good habit we’ve got into."
Prof Oxford said that the Covid-19 vaccines tended to have "much better coverage of variants" than influenza vaccines. He said, however, that the need to continue to be vaccinated varied from person to person.
"If they’re extremely busy and 25, maybe don’t have time, I can understand that [they may not get vaccinated]," he said.
"If you’re 55 and maybe had a touch of bronchitis, you’re in a vulnerable group and should continue with the vaccination. The older you are, the more vulnerable."
Prof Hunter said he thought that a vaccination programme that focused on more vulnerable groups was appropriate, saying that most people in the UK, for example, will have had previous infections, which will confer some immunity in the event of subsequent infection, as will previous vaccination.
According to Prof Jones, there is "questionable" need for vaccine updates for "an average member of the population", with Covid-19 now presenting as "a mild cold-like infection" in such individuals.