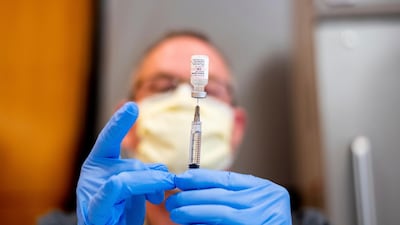
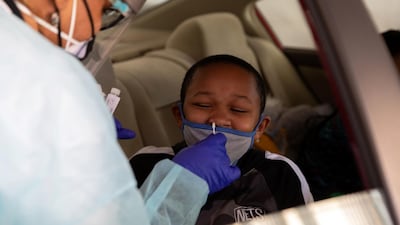
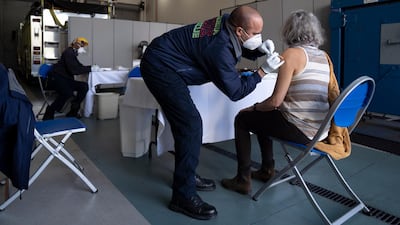
The intensive care rooms at St Luke's Boise Medical Centre are full, each a blinking jungle of tubes, wires and mechanical breathing machines. The patients nestled inside are a lot alike: all unvaccinated, mostly middle-aged, paralysed and sedated, reliant on life support and locked in a silent struggle against Covid-19.
But watch for a moment and glimpses of who they were before the coronavirus become clear.
Artfully inked tattoos cover the tanned forearm of a man in his 30s. An expectant mother's slightly swollen belly is briefly revealed as a nurse adjusts her position. The young woman is five months pregnant and hooked to a breathing machine.
Down the hall, another pregnant woman, only 24 and hooked to a ventilator, is lying prone — on top of her developing foetus — to bring more air into her ravaged lungs.
Idaho hit a grim Covid-19 trifecta this week, reaching record numbers of emergency room visits, hospital admissions and ICU patients. Medical experts say the deeply conservative state is likely to record 30,000 new infections a week by mid-September.
With a critical shortage of hospital beds and staff and one of the nation's lowest vaccination rates, Idaho health providers are growing desperate and preparing to follow crisis standards of care, which call for giving scarce resources to patients most likely to survive.
St Luke's Boise Medical Centre invited The Associated Press into its restricted ICUs this week in hopes that sharing the dire reality would prompt people to change their behaviour.
“There is so much loss here, and so much of it is preventable. I'm not just talking about loss of life. Ultimately, it's like loss of hope,” said chief medical officer Dr Jim Souza. “When the vaccines came out in December, those of us in health care were like, 'Oh, my God, it's like the cavalry coming over the hill … To see now what's playing out? It's all so needless.”
Inside the ICUs, Kristen Connelly and fellow nurses frequently gather to turn over each patient, careful to avoid disconnecting the tangle of tubes and wires keeping them alive. With breathing tubes, feeding tubes and half a dozen hanging bags of medications intended to halt a cascade of organ damage, turning a patient is a dangerous but necessary endeavour that happens twice a day.
When Idaho’s hospitals were nearly overwhelmed with coronavirus patients last winter, Ms Connelly wasn’t disconcerted, believing she could make a difference. Now, instead of focusing on one patient at a time, she cares for multiple. Many colleagues have quit, burnt out by the relentless demands of the pandemic.
“At this point, I’m overwhelmed. I don’t have much left,” the 26-year ICU nursing veteran said on Tuesday.
Ms Connelly’s own life is in triage mode as she tries to maintain her last reservoirs of energy. She doesn’t eat at home any more and has cut out all activities except for walking her dog. Her normally deep sense of compassion — which Ms Connelly considers a critical job skill — has been shadowed by a seething anger she can't shake.
“We had a mother-daughter team in the hospital last week, and the mother died and the daughter was still here,” Ms Connelly said. “In that moment, I had a reprieve from the anger, because I got to be just overwhelmed with sadness.”
“It’s devastating,” she said. “Where we are right now is avoidable — we didn’t have to go here.”
All of the ICU coronavirus patients were generally healthy people who simply weren't vaccinated, Dr Bill Dittrich said. Idaho could enact crisis care standards in days, leaving him to make gut-wrenching decisions about who receives life-saving treatment.
“I don’t think anybody will ever be ready to have the kinds of conversations and make the kinds of decisions that we’re concerned we’re going to have to be making in the next several weeks. I’m really terrified,” Mr Dittrich said.
ICU nurse
Most of the ICU patients fell prey to con-artists before they fell ill with the virus, said Dr Souza, the chief medical officer. He points to a patient who first tried the anti-parasite drug ivermectin. US health officials have said it should not be used to treat Covid-19. The man, in his 50s, refused standard medical treatments until he became so sick he needed to be admitted.
“What we’re left with is organ supportive therapy. Misinformation is hurting people and killing people,” Dr Souza said.
What the science is clear on? Vaccines, he said. “We don't have any vaccinated patients here.”
In deep-red Idaho, however, vaccinations, masks and nearly anything related to the coronavirus marks a de facto borderline between more traditional Republicans and the far-right.
Republican Governor Brad Little urged residents this week to show love for their neighbours by being vaccinated and announced he was using federal programmes and mobilising the Idaho National Guard to bring in hundreds of additional healthcare workers. In response, Lieutenant Governor Janice McGeachin called the statement “shameful".

Ms McGeachin, who is running against Mr Little in the Republican gubernatorial primary, and who has tried to bar schools and cities from enacting mask rules, said people should make their “own health choices".
The rift exists at the local level, too. Ada County commissioners voted to nominate a local pathologist to a regional public health board who has referred to Covid-19 vaccines as “needle rape” and the “clot shot”. Dr Ryan Cole's appointment still depends on votes by other county leaders.
Even families who have witnessed the trauma of Covid-19 first-hand are on opposite sides.
Lisa Owens's 48-year-old stepbrother, Jeff Owens, has been in the Boise hospital's ICU since early August.
“My kids call him the ‘Candy Man’ because he always brings candy when he comes,” Ms Owens said. “He really is this kind, loving, jovial person, and I wish with all my heart that he’d got vaccinated.”
She's vaccinated, along with about half of her extended family. But Jeff Owens, their aunt and uncle, Jeff’s daughter and a few others are not. Her stepbrother likely caught Covid-19 from the aunt and uncle, Ms Owens said. The aunt was admitted to hospital — she developed blood clots from the virus — but has since recovered.
If anything, those experiences entrenched other relatives in their anti-vaccination beliefs, Ms Owens said.
“Sure, they see Jeff in the hospital, but they also see his aunt and uncle, and they’re OK. The last update we had is even if he does recover, he’s looking at eight months of rehab,” she said. “If he pulls through, I’m going to march him into the nearest vaccine clinic myself.”
Ms Owens fears her stepbrother may be taken off life support if someone with a better chance of survival needs the bed.
“I don’t even want to think about it. … I mean, he’s been in there for a month. If it comes to crisis standards of care, they’re going to say he’s not showing enough improvement, because he’s not,” she said, fighting back tears. “I hope he pulls through it.”