This world war has been raging for more than a century. Its casualty rate now runs into the millions. Tens of thousands have died, while many more have been blinded and crippled. But, finally, the day of victory may be at hand.
The enemy is polio, a virus which can kill up to one in three of those who exhibit symptoms and leaves others paralysed or without sight. It has existed for centuries, but it became a scourge in the early years of the last century, spread through poor sanitation in fast-growing urban areas.
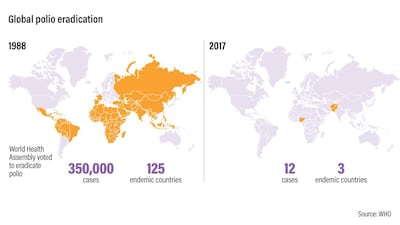
This Tuesday is World Polio Day, an anniversary that marks the continuing fight against the disease. Even 30 years ago, polio was endemic in more than 125 countries on almost every continent. At least 300,000 people caught the disease in 1988, although life-saving vaccines have been in use since the 1950s.
This year, just 12 people have been diagnosed with polio, a historic low. The disease exists in only two countries, Pakistan and Afghanistan. With the transmission season almost over, this total is unlikely to rise significantly.
Last year, 37 people caught wild polio, all in those two countries. An outbreak in Syria in 2014 has been contained. Fingers are crossed for Nigeria, polio free for two years until two cases were reported in August 2016, but nothing this year.
If these trends continue, like the disease itself, World Polio Day will very soon become a thing of the past.
The impending victory over polio will be marked next month in Abu Dhabi at Reaching the Last Mile, a landmark forum jointly hosted by Sheikh Mohammed bin Zayed, Crown Prince of Abu Dhabi and Deputy Commander of the Armed Forces, the Bill and Melinda Gates Foundation, and the Carter Centre, founded by former US president, Jimmy Carter.
It will be marked, but there will be no time for celebration.
For while the day approaches when polio will be driven from the world, a far more terrible war still rages. This conflict destroys around 400,000 lives every year. More than nine out of 10 who perish are children.
_______________
Read more:
Sheikh Hamed opens Countdown to Zero: Defeating Disease global exhibition in Abu Dhabi
UAE pushes for political commitment to eradicate preventable infectious diseases
_______________
As polio faces defeat, so attention turns to malaria. The agenda of Reaching the Last Mile will reflect this. The UAE has long funded and supported efforts to eradicate polio. Only last month, the office of the Crown Prince announced US$5 million more in funding, but this time for malaria.
“This is a preventable disease,” says Dr Maha Barakat, of the Department of Heath. Around 90 per cent of all cases of malaria are found in Africa, and of these 92 per cent are children.
Ninety-five per cent of lives saved as a result of scale-up malaria interventions between 2000 and 2015 are in the under-five age group.
“Malaria costs African countries $12 billion every year.” Dr Barakat says. “If I told you that the amount we need to completely finish the fight is about $6bn, that puts it into perspective. Six billion dollars seems a lot of money until you compare it with what Africa alone pays.”
What offers hope is that other diseases, once widespread, have been, or are about to be eradicated. Smallpox, which killed two million people as recently as 1967, was wiped out by 1980.
In 1990, Sheikh Zayed made the first donation to the Carter Centre, with the goal of eradication Guinea worm disease, the cause of blindness across large areas of Africa.
“In 1986, there were three-and-a-half million cases of guinea worm in the world,” says Dr Barakat.
“This is a disease for which there is no vaccine, no treatment. It’s a debilitating disease
“Now there are only a handful of cases in the world and in one country only, and that’s Chad. So we are almost there. It’s a 99.999 per cent reduction in this disease and we are really, really very close to eradicating it.”
A more sophisticated approach to disease management is the key to final eradication, says Dr Chris Elias, president of the Global Development Programme at the Gates Foundation.
“If you look at the eradication successes in smallpox, and now guinea worm and polio, you tend to make rapid progress in many places and then the last few places are quite challenging often because they have specific and unique challenges,” he says.
These include populations that are difficult to reach, security issues that can make it dangerous for health works and even communities that refuse vaccines because they believe they are a western plot.
In Afghanistan and Pakistan, the Taliban spread rumours that the polio vaccine was designed to sterilise children in a plot to eradicate Muslims. Dozens of health workers have been murdered in these areas as a result.
Deploying Muslim health workers from organisations like the Emirates Polio Campaign has been one way of successfully reassuring these populations.
There are other challenges. Some of the most vulnerable populations to polio are migratory. Detecting the wild polio virus in water and sewage becomes more difficult as the disease declines.
Campaigners now study migratory patterns and deploy ever more sophisticated environmental monitoring equipment. Even success can cause problems, as Dr Elias explains.
“As the number of cases gets smaller, then the amount of money you need to spend on each case goes up and explaining that can be a challenge," he says. “What worked to reach most people isn’t going to reach the last people.”
Roll Back Malaria is a key international partnership in fighting the disease. It is a sign of the larger efforts that the name of the organisation is amended to Roll Back Malaria For A Malaria Free World.
There are targets. A 40 per cent reduction in deaths by 2020, rising to 70 per cent by 2025 and 90 per cent in 2030. It may seem an ambitious target, but can be seen in the context of a halving of the death rate since 2000, when malaria killed nearly a million a year. Viewed another way, it translates to around six million people, mostly children, who would otherwise be dead.
Reaching this last mile, Dr Elias explains, will be even more complex than eradicating polio. There is just one vaccine, newly developed through the support of the Gates Foundation, but is still undergoing trials, and appears to be less effective with the most vulnerable — very young children.
One of the challenges is that the malaria parasite is very complex and is constantly trying to evolve resistance against the drugs, says Dr Elias. “So, in addition to deploying the tools we have, we have to keep investing in the research and development of new drugs.”

Some of the most promising research is into so-called “transmission blocking vaccines” which can be given to humans but would act on the disease-carrying parasites that live in the gut of mosquitos.
In other areas, the solutions are cheaper and more effective. More effective insecticide to kill mosquitos, chemically treated nets for bedding that now last three years rather than one, faster and cheaper diagnosis and treatment.
If malaria can be obliterated from the face of the planet, it will be one of mankind’s greatest achievements. But the task will not be easy. Nor is there room for complacency.
Even in its apparent death throes, polio still lurks, waiting for an opportunity. “If we stopped all prevention efforts, the number of new polio cases would jump about 200,000 around the world every year,” says Dr Barakat. “We’re not just talking about two or three countries; we are talking about re-emergence in the whole world.”
The last case of polio in the UAE was reported in 1992, with the country declared free of the disease in 2004. Locally contracted cases of malaria have not been seen since 1997, with the UAE declared malaria free by the WHO in 2007.
But it is not enough for any one country to say that because they are free of these diseases they can push it down the political agenda, says Dr Barakat.
Governments need to keep funding as a top priority, she says, adding: “We need funding to get to the last mile.”