Thin-looking people may be just as susceptible to heart disease and diabetes as the obese according to a study of fat distribution in more than 6,000 patients.
Researchers have found traditional indicators of obesity such as body mass index (BMI) may not be giving a clear indication of health, with thin people also vulnerable to storing harmful fat deposits internally.
BMI, or Quetelet index, is a value defined as the body mass divided by the square of the body height in units of kg/m2, with scores under 18 commonly viewed as underweight, and those over 25 over weight.
However, the rating does not consider overall build and muscle mass.
Results of the joint study between Westminster University, Linköping University, pharmaceutical company Pfizer and body composition analysts AMRA suggest finding specific patterns of fat distribution in patients is a more effective way of managing metabolic conditions.
“By using an intuitive visualisation of body composition, we’ve been able to identify a wide range of body composition profiles that could provide the link to increased risk of metabolic diseases,” said Dr Olof Dahlqvist Leinhard, a senior author of the study.
AMRA, a digital medical company, performed an automated analysis of MRI images for precise fat and muscle measurements, and has developed a technique for body composition profiling. It allows doctors to analyse detailed links between fat, muscle and a patient’s metabolic status.
Specific fat distribution patterns can indicate heart disease and diabetes according to the Swedish scientists who looked at the body composition of more than 6,000 people.
The results of the study have shown how personalised healthcare could develop in future, leaving behind traditionally used perceived health markers like BMI readings.
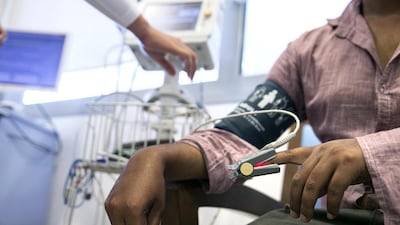
Experts at the Canadian Specialist Hospital in Dubai said multiple measures should be taken to make an accurate assessment of a patient’s risk level to metabolic disease.
“BMI should not be used as a sole indicator to metabolic diseases,” said Alaa Takidin, a clinical nutritionist at the hospital.
“We have come across patients with different weights, gender, age and percentage body fat having the same BMI. There are so many other indicators that should be used in conjunction with a BMI reading to have a complete picture of a body composition and risk of metabolic disease.”
Doctors at the facility asses a patient by gathering information about their past medical history, family history, three-day dietary recall, smoking and alcohol intake and their level of physical activity.
They also look at anthropometric measures such as skin fold tests, water intake and the patient’s highest and lowest weight for the past five years. Body fat percentage, muscle mass, total calorie intake and water mass are also assessed to evaluate patient health.
“Visceral fat or internal fat is a specific type of fat that is found on the stomach, with high visceral fat dangerous and correlated with cholesterol, diabetes, Alzheimer’s and other health conditions,” said Ms Takidin.
“There are many ways to measure visceral fat which include CT scans, bioelectrical impedance machines and waist to hip circumference.”
The findings lend further support to the value of more detailed health evaluations to determine suitable lifestyle change or medical care, such as those delivered by the Bodyo health pods currently under trial with Dubai Health Authority, as The National reported earlier this year.
Bodyo’s health analysis AiPods were selected by DHA to create solutions for problems facing society as part of the Dubai Future Accelerators programme.
____________________
Read more:
Science: Skinny people could be just as unhealthy as those who are overweight
Health pods installed in Dubai government offices will collect workers' data
Biohacking explained: meet the group who practise in the UAE
Long-term diabetes study to identify risk factors in UAE
_____________________
The pods detect a multitude of health signals, bodyfat, bone mass, muscle mass, hydration, intracell and extra cells hydration and metabolic age. They are now being widely used in several government departments and could indicate how healthcare could be better managed in future.
"Sensor inside the pod are our own and are due to be patented," said Bodyo founder Patrice Coutard.
"It allows us to give results and with our algorithms, recommend personalized food supplement needed and nutrition plans.
"We are working to implement our existing product to give the distribution per segment and assess visceral fat via a 3D model."
Other elements to measure health are through the appearance of skin, signs of hair loss, stress or body fatigue level, decreased cravings, irregular bowel movements, overall mood and strength of the immune system.
Mabina Daniel Lengweng, who runs a personal training business in Dubai, said results from BMI measurements can often be misleading and should not be relied on as a sole indicator of good health.
His company, Vigour Energy, also checks blood pressure, glucose level, waist to hip ratio, skin fold measurements, MRI scans and hydrostatic weighing to understand someone’s health level status.
“BMI is a complex method which could be confusing to individuals and may lead them to believe they are overweight or obese even when they are in good shape,” he said.
“Personally, I do not follow BMI as it sometimes classifies a lean person as overweight due to high body fat percentage”


