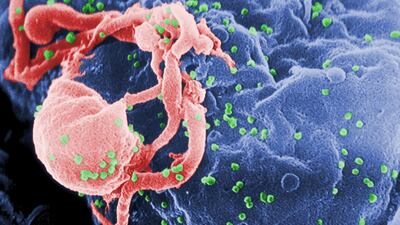
An HIV-positive man in Britain has become the second known adult worldwide to be cleared of the AIDS virus after he received a bone-marrow transplant from an HIV resistant donor, his doctors said.
Almost three years after receiving bone marrow stem cells from a donor with a rare genetic mutation that resists HIV infection — and more than 18 months after coming off antiretroviral drugs — highly sensitive tests still show no trace of the man's previous HIV infection.
"There is no virus there that we can measure. We can't detect anything," said Ravindra Gupta, a professor and HIV biologist who co-led a team of doctors treating the man.
The case is proof of the concept that scientists will one day be able to end Aids, the doctors said, but does not mean a cure for HIV has been found.
Mr Gupta described his patient as "functionally cured" and "in remission", but cautioned: "It's too early to say he's cured."
But the International Aids Society (IAS) welcomed the news, saying it may help scientists searching for a cure.
"The hope is that this will eventually lead to a safe, cost-effective and easy strategy to achieve these results using gene technology or antibody techniques," said IAS President Anton Pozniak.
The man, who does not want to be named, is being called "the London patient", in part because his case is similar to the first known example of a functional cure of HIV – in an American man, Timothy Brown.
Mr Brown is also known as the second 'Berlin patient' when he underwent similar treatment in Germany in 2007 which also cleared his HIV. Mr Brown moved to Berlin after a still unnamed patient received experimental therapy in 1998. While Mr Brown is HIV-free, the first Berlin patient has maintained low levels of HIV even though he has remained off anti-retroviral therapy.
Some 37 million people worldwide are infected with HIV and the Aids pandemic has killed around 35 million people since the 1980s. Scientific research into the complex virus has in recent years led to the development of drug combinations that can keep it at bay in most patients.
Mr Gupta had treated the London patient when he was working at University College London. The man had contracted HIV in 2003, Gupta said, and in 2012 was also diagnosed with a type of blood cancer called Hodgkin's Lymphoma.
In 2016, when he was very sick with cancer, doctors decided to seek a transplant match for him. "This was really his last chance of survival," Mr Gupta said.
The donor – who was unrelated – had a genetic mutation known as 'CCR5 delta 32', which confers resistance to HIV.
The transplant went relatively smoothly, Mr Gupta said, but there were some side effects, including the patient suffering a period of "graft-versus-host" disease, a condition in which donor immune cells attack the recipient's immune cells.
Most experts say it is inconceivable such treatments could be a way of curing all patients. The procedure is expensive, complex and risky. To do this in others, exact match donors would have to be found in the tiny proportion of people – most of them of northern European descent – who have the CCR5 mutation that makes them resistant to the virus.
Specialists said it is also not yet clear whether the CCR5 resistance is the only key or whether the graft-versus-host disease may have been just as important. Both Brown and London patients had this complication, which may have played a role in the loss of HIV-infected cells, Mr Gupta said.
Sharon Lewin, an expert at Australia's Doherty Institute and IAS co-chair of their cure research advisory board, told Reuters the London case points to more avenues for study.
"We haven't cured HIV, but [this] gives us hope that it's going to be feasible one day to eliminate the virus," she said.
Gupta said his team plans to use these findings to explore potential new HIV treatment strategies. "We need to understand if we could knock out this [CCR5] receptor in people with HIV, which may be possible with gene therapy," he said.
The London patient, whose case was set to be reported in the journal Nature and presented at a medical conference in Seattle on Tuesday, has asked not to also reveal his age, nationality or other details.