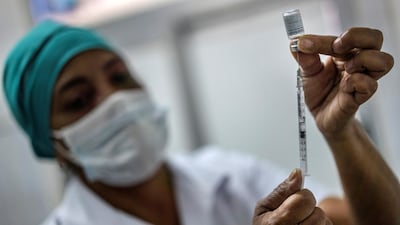
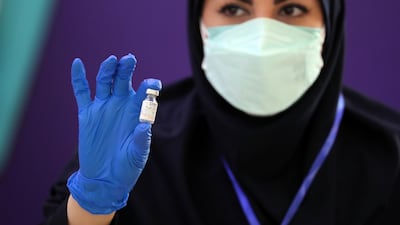
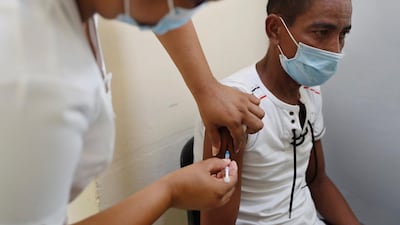
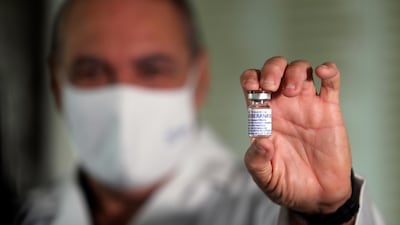
A next-generation Covid-19 vaccine is primed to join the global fight against the pandemic.
With several highly effective shots already widely introduced in countries around the world, the chances for other vaccines to play a major role in combating the pandemic may be narrowing.
However, of the more than 250 shots being worked on but not yet approved, some have a better chance of making an impact than others.
Among the most promising is an inactivated whole virus vaccine from Valneva, a French biotechnology company. The UK government has ordered 100 million doses, production has begun at a factory in Scotland and the first doses should be delivered later this year, if the shot is approved by regulators.
David Lawrence, the company’s chief financial officer, said the technological approach taken meant the vaccine “has an important role to play”.
“The world needs multiple vaccines, as well as booster options, and our vaccine would help diversify the overall portfolio," he said.
Efficacy of vaccines compared in trials
The vaccine, called VLA2001, consists of coronavirus particles treated so they cannot cause disease. It also contains an adjuvant, a substance to strengthen the immune response, produced by Californian company Dynavax Technologies.
It is the only Covid-19 vaccine taking this approach to be in clinical trials in Europe and is involved in two studies expected to report results in September.
Cov-Compare, a UK study involving 4,000 participants, pitches the vaccine against the Oxford-AstraZeneca shot, with the immune response to each vaccine compared two weeks after the second shot.

At this stage of the pandemic, a clinical trial comparing the vaccine against a placebo would have been “infeasible and ethically highly questionable”, Mr Lawrence said.
The shot, which could be used as a booster or as a main vaccine, is also part of Cov-Boost, a clinical trial of seven vaccines to measure their effectiveness at improving the immunity of already vaccinated people.
“It is the first trial in the world to provide vital data on how effective a booster of each vaccine is in protecting individuals from the virus," said Mr Lawrence.
Data reported in April from earlier-stage trials showed the vaccine “was well tolerated, with no safety concerns identified, and highly immunogenic”.
New approach to a time-honoured method
Later trial data will determine whether final regulatory approval is forthcoming. Inactivated vaccines are longer established than the mRNA vaccines, such as the Moderna and Pfizer-BioNTech shots, and viral vector vaccines such as the Sputnik V and Oxford-AstraZeneca shots, that are proving effective against the disease.
The first were made in the late 19th century in the US and France, and they have been used against influenza, hepatitis A, polio and rabies. The pathogen is grown in culture and inactivated or killed by, for example, heat or chemical treatment, so that while the vaccine stimulates an immune response that protects against disease, the shot itself does not cause illness.
Paul Hunter, a professor in medicine at the University of East Anglia and specialist in infectious diseases, described inactivated vaccines as “established technology”.
“I was quite surprised the West didn’t put a lot of effort into inactivated vaccines early on because you could pretty much guarantee they would work, but we went for the more technologically exciting vaccines”, he said.
Given the high efficacy of the Moderna, Pfizer-BioNTech and Oxford-AstraZeneca shots, that approach appears to have been vindicated.
Vaccine market continues to grow:
But Mr Lawrence said inactivated whole virus vaccines had several benefits, including their ability to be modified to cope with new variants, and their effectiveness as repeat booster vaccinations.
Valneva has “viral seed banks” that include the Alpha and Beta strains of Covid-19, so variant-based vaccines can be produced.
“[Inactivated vaccines] can be used in people with weakened immune systems – for example those who are at greatest risk from Covid-19 – and routinely conform to standard cold-chain requirements, which makes them easier to store and distribute," said Mr Lawrence.
Sinovac and Sinopharm in China and India’s Bharat Biotech have produced inactivated Covid-19 vaccines.
Vaccine producer with invaluable experience
Headquartered in Saint-Herblain, a suburb of the city of Nantes in western France, Valneva was founded in 2013 after the merger of a French and an Austrian company.
A vaccine specialist, it has two approved shots, against cholera and Japanese encephalitis, and aside from the Covid-19 vaccine, two under development, to combat Lyme disease, a bacterial condition spread by ticks, and chikungunya, a viral disease mosquitoes carry.
Mr Lawrence said Valneva began producing VLA2001 at its site in Livingston, Scotland, in January, and additional capacity will come on stream in the second half of this year with financial help from the British authorities.
“Alongside this, we are investing in our site in Solna, Sweden, to expand capacity for our inactivated Covid-19 vaccine," he said.
Delivery of the first 60 million of the 100 million doses ordered by the British government is scheduled to continue into the first quarter of next year, with the rest also due for delivery in 2022.
The UK authorities have options for a further 90 million doses to be delivered between 2023 and 2025 that would bring the total value of the order up to €1.4 billion ($1.6bn).
“The question is, who’s it for, because we’ve ordered more than enough Pfizer vaccine to vaccinate everyone [in the UK] in the autumn. I suspect we’ve done it so we can get it up and running and donate it or sell it to other countries down the line," said Prof Hunter.
The vaccine’s stability means it could, experts have said, be useful for western governments looking to stockpile supplies. Equity research analysts Jefferies has suggested the vaccine could bring in $1.1bn for Valneva next year and a further $500m in 2023, Fierce Pharma reported.
These are significant sums, but a fraction of those set to be earned by, for example, the Moderna and Pfizer-BioNTech shots. Valneva is hoping to strike new deals in addition to those it has with the UK. Reports have suggested France, Germany and Sweden are possible buyers after an EU-wide deal was not completed.
“We are speaking with various governments," said Mr Lawrence.
“We believe that our inactivated vaccine can make a major contribution to the ongoing fight against the pandemic and remain committed to bringing it to market.”