As this winter’s flu epidemic increases its grip, it’s hard not to feel a frisson of panic the instant you feel under par.
You know the symptoms: tiredness, perhaps a headache or cough, then aching joints – and a fever.
And for most of us, the standard advice is simple: go to bed, stay hydrated, and take paracetamol or something similar to deal with the aches and fever.
Forget miracle-cures. Antibiotics are useless against a viral disease like influenza, and anti-virals come with no guarantee of efficacy. Your best hope lies in your own disease-fighting immune system, which will typically cure you in around a week.
But among medical scientists, there’s growing concern that the standard advice may actually undermine our own defences - with potentially lethal consequences.
Their scepticism stems from evidence that we may have misunderstood fever, which may in fact be one of our body’s most potent weapons against infection.
As such, quelling it using paracetamol and the like may be a really bad idea.
On the face of it, fever is obviously a bad thing – something cooked up by germs to wreak as much havoc as possible.
Yet for most of medical history, fever has been regarded as beneficial – even something to be encouraged.
Not until the mid-19th century did attitudes change, with the emergence of a “scientific” approach to medicin
___________
Read more on Science
Vaping remains off the table in UAE for New Year resolutions
Key to cancer may lie within our own bodies, but fears grow that wonder drugs will be elite-only
___________
Physicians came to think of the human body as a kind of machine, equipped with a set of checks and balances to keep it healthy.
Deviations from normal conditions – including increased body temperature - were seen as indicators that something was wrong with the body’s machinery and needed to be fixed.
By the start of the 20th century, fever could both be diagnosed – thanks to the invention of the medical thermometer- and also remedied, using the new wonder-drugs aspirin and paracetamol.
Soon doctors were presented with a golden opportunity to use these breakthroughs to help humanity on a global scale.
Almost exactly a century ago, the mother of all influenza outbreaks – the so-called Spanish Flu pandemic – reared its head. Over the next year it infected of 500 million and killed an estimated 50 to 100 million – around 4 per cent of the world’s population.
Doctors swung into action, using the new “antipyretics” like aspirin to help combat fever.
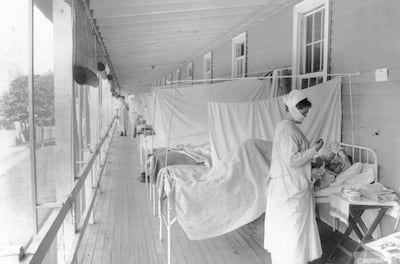
Yet while they doubtless believed they were benefiting their patients, evidence emerged pointing to a darker conclusion.
Statistics showed that patients given the fever-busting aspirin died in far higher numbers than those treated with homeopathy, widely regarded by many doctors as equivalent to given patients nothing at all.
Such anecdotal reports were swept aside by the march of medical science.
The advent of antibiotics in the 1940s and then anti-virals made the idea of “sweating out” an infection seem quaint and ill-advised.
But now it is being taken seriously once more, as supporting evidence emerges from an impressive array of disciplines.
Studies of bacteria and viruses have revealed that high temperature can undermine their ability to replicate, with concentrations plunging after being held at a fever-like 40C for several hours.
Meanwhile, immunologists have found that many of the disease-fighting cells in the human immune system work more effectively during fevers.
Nor are humans alone: biologists have found that mammals, birds, fish and even reptiles are all equipped with fever-producing systems.
According to a recent review of the evidence in the journal Nature, it seems living organisms have used fever to combat infection for at least 600 million years, and possibly longer.
It also appears to be strikingly effective. A 2010 study of patients admitted to UK hospitals with non-severe pneumonia showed that those with the worst fevers had the lowest risk of death.
But evidence has also emerged backing the flip-side: that taking drugs to combat fever is not just misguided, but potentially fatal.
Studies of animals infected with influenza showed that those given fever-breaking “antipyretics” like aspirin and paracetamol have found that the treatment typically increases the risk of death.
The same seems to be true with humans. In a pioneering clinical trial on humans published in 2005, Dr Carl Schulman of the University of Miami found that patients given fever-busting drugs were over six times more likely to die than those left to sweat it out.
So dramatic was the difference that the trial was stopped on ethical grounds.
Despite this, many doctors and patients remain convinced that, whatever its benefits, fever is not always best left untreated. The higher temperature puts strain on the metabolism, and can run out of control with some conditions, with potentially fatal results.
The need for caution was highlighted by a recent Korean-Japanese study of the effect of fever among almost 1,500 critically ill patients. Patients with sepsis – infection-related - fever were much more likely to survive when it left untreated, compared to those given antipyretics.
In contrast, patients without sepsis did far worse if their fever was left alone.
Overall, the evidence points to fever being a key part of the body’s ability to fight infections.
Despite this, anyone with flu will find it hard to resist the temporary respite offered by drugs like paracetamol. Yet research suggests that, in the case of influenza at least, this may not only prolong the misery but also help spread the infection.
Put simply, the treatment fools people into thinking they’re cured and able to get back to their lives, thus exposing others to the virus.
In 2014, a team led by David Eam at McMaster University, Canada, analysed data on flu epidemics and found the use of antipyretics may boost the death-toll by around 3 per cent – simply by allowing people spread their infection.
They point out that this unintended consequence of treating fevers could have boosted the scale of the 1918-19 pandemic. The miracle-cure of aspirin may have increased the death-toll by perhaps several million.
Given such statistics, and the risk of another flu pandemic on a similar scale, one might think public health organisations would be racing to understand more about the benefits of fever. Yet to this day, the 2005 University of Miami study remains the only randomised controlled trial designed to give reliable insights.
Until more insights are forthcoming, the standard advice remains in place: rest, stay hydrated and take paracetamol and the like to manage the aches, pains and fever. And if you don’t feel better within a week, seek medical help.
It's advice that would be more reassuring if it included some hard science about the benefits of “sweating it out”.
Robert Matthews is Visiting Professor of Science at Aston University, Birmingham, UK

