It could take up to four years to vaccinate the global population against Covid-19, a major drug maker said.
Zydus Cadila, a company in India, said it would take time to ensure effective and affordable vaccines were available worldwide.
The company's managing director told The National that there may need to be an annual immunisation programme – like the flu shot – to top up people's resistance and as strains mutate.
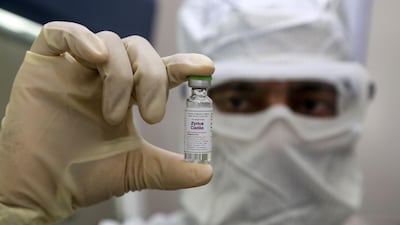
Zydus Cadila's ZyCoV-D is among dozens of potential vaccines being developed worldwide.
Dr Sharvil Patel, managing director of Cadila Healthcare, said the company was on track to have its own vaccine available by June.
The drug maker is also repurposing existing medicine to treat Covid-19 patients who could suffer from long-term damage to their lungs, kidneys and liver.
“I strongly believe there would be more than a few vaccine manufacturers,” said Dr Patel, 41, from the company’s headquarters in Ahmedabad, western India.
“If we are talking about numbers for India, we need at least a billion-plus doses which is not practically possible over a short time.
“There will be demand at least for the next three to four years for the vaccine.
“This could become an annual jab one needs to take, part of overall immunisation like the flu vaccine.”

Cadila is one of two Indian drug makers working to develop an indigenous Covid-19 vaccine.
It is preparing to produce more than 100 million doses a year, plus an additional 50 to 70 million doses with partners once trials are successfully completed.
About 30,000 volunteers will receive injections in India next month as part of final-stage trials.
Data from second-phase human trials on 1,000 people will be released in a few weeks.
"We are looking for a good result for Phase 2 that we will know by end of the month," he said.
“We are already in preparation for a large Phase 3 trial for 30,000-plus volunteers that we hope to commence in December.
"We are looking at the April-June quarter when the vaccine could be available.”
Among the country’s top drug makers by revenue, Cadila also produces other coronavirus treatments such as remdesivir.
ZyCoV-D is being developed in Ahmedabad and vaccine research is also being conducted in Italy.
The company has already identified manufacturers they will work with to produce the vaccine for overseas markets.
“Ours does not require a highly specialised contained facility so it’s relatively easier to set up,” said Dr Patel.
“It will definitely be the Middle East region, North Africa, South-East Asia and Latin American markets,” he said.
“If the data is very good we will look at European and other developed markets including Australia and others. Currently our visibility is between 100 to 170 million doses – that is what we will prepare for.”
This month, Moderna and Pfizer each announced that their vaccines were between 90 and 94 per cent effective. But both require refrigeration at minus 20°C and minus 75°C, posing logistical issues for distribution.
For developing countries such as India, with a population of 1.3 billion, a vaccine would need to be mass-produced with low cold-chain storage requirements.
Pricing will be critical for countries that are not able to manufacture vaccines themselves.
Dr Patel said ease of delivery would be vital. Cadila’s DNA-based vaccine needs to be stored at between 2°C and 8°C.
“The thermal stability is challenging for many of the developed vaccines,” he said.
"The vaccine platform we have developed is far more manageable for distribution and logistics."
Conventional vaccines use weakened or killed versions of a virus. Gene-based DNA vaccines take a small part of the virus’ genetic information – enough to trigger an immune response – to prompt production of proteins directly in the cell to fight the virus.
Dr Patel said a substantial portion of the world’s population would continue to require treatment for Covid-19 until large-scale vaccination was ready.
“You do see issues related to kidney, lung and liver damage. Severely affected patients get into acute respiratory distress syndrome because of large damage to the epithelial cells of the lungs so you would definitely need treatment when people are in that stage,” he said.
“We are developing and repurposing some of our drugs that can treat some of these underlying conditions of the virus.
“We are trying to repurpose medicines to reduce the viral load early on so we don’t require hospitalisation or at least reduced oxygen.”
India is known as the "pharmacy of the world" for producing cost-effective drugs – a lifeline in countries that cannot pay high prices to treat illness such as HIV, asthma and cancer.
Dr Patel said India would continue to play this role during the pandemic.
“Not only are we working on research to fight [Covid-19], we want to contribute in making drugs available and affordable,” he said.
Dr Patel, the third-generation head of a family-owned business, said the pandemic taught people to look out for the vulnerable population and the elderly.
“This is something that it is important for everyone to understand. You don’t have to only be worried for yourself. You have to worry about people who you may infect if you are not careful," he said.