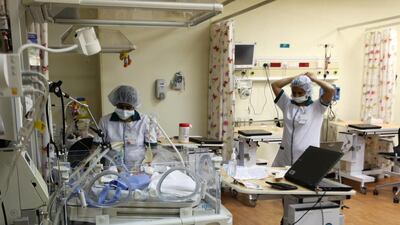
ABU DHABI // Health experts are calling for better measures in hospitals to prevent the spread of the deadly Mers coronavirus disease.
They said that, while hospitals have taken steps to prevent clusters of the disease breaking out, further measures were needed to improve hygiene, such as making visitors thoroughly wash their hands, special air filters and providing protective clothing to staff.
Health officials are to discuss the issue of environmental decontamination at the Patient Safety Middle East Exhibition and Conferences in Dubai, that will take place from September 16 to 18.
Among the speakers will be Dr Mushira Enani, head of infectious diseases at King Fahad Medical City in Saudi Arabia, who will be outlining patient-safety difficulties concerning Mers.
When the Mers outbreak hit Saudi, the country’s health service was criticised over its hygiene measures, which were facilitating the spread of the disease.
Dr Enani said changes had been made, both in Saudi and other GCC countries, to manage the disease. She said hospital staff had been reminded about ways to control infection to make sure the disease was contained, but more needed to be done.
“In my opinion, the top patient safety dilemmas in 2014 are lack of infection prevention and control, as well as environmental hygiene,” she said.
“In particular, hand hygiene is still suboptimal in many healthcare facilities in the region contributing to the spread of superbugs, and emerging viruses to patients. Consequently this is jeopardising their safety.
“Mers-CoV clusters within hospitals were triggered by poor practise of infection prevention that lead to a surge of the virus in multiple hospitals in the Arabian Peninsula.”
She added that many hospitals lacked facilities such as negative pressure rooms and high-efficiency particulate air (Hepa) filters, which were crucial to prevent the virus spreading by air.
Dr Ulrich Wernery, a director at the Central Veterinary Research Laboratory in Dubai who conducted a study on Mers, agreed improvements in hygiene practices had been necessitated by Mers.
“The transmission rate of the infection between people [in hospitals] has dropped tremendously,” he said.
“This is because hospitals have been careful about maintaining good hygiene and medical staff have been cautious. Also, people have become aware and wash their hands more and more, and this is helps in controlling the spread of the disease.”
He said another important way to manage infections was through diagnosis.
Many hospitals had now introduced the Polmerase Chain Reaction (PCR) test, a highly sensitive test that can detect small amounts of genetic material in samples of blood, tissue or body fluids.
Results could be announced much quicker than sending samples to a regional laboratory and waiting several days.
So, if anyone was diagnosed with Mers, they could be isolated and treated straight away.
According to the World Health Organisation (WHO), transmission of Mers had occurred in healthcare facilities in several countries, including from patients to healthcare workers.
It was not always possible to identify patients with Mers coronavirus early or without testing because symptoms and other clinical features might be non-specific. For this reason the WHO said it was important that healthcare workers applied standard precautions consistently with all patients.
arizvi2@thenational.ae