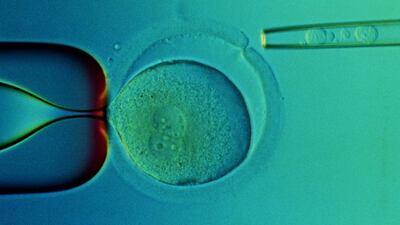
It is easy to understand why someone would try anything and spend any amount of money to save their lives, but the list of diseases for which stem cell treatments have been shown to be beneficial is still very short.
For decades, stem cell treatment has been hailed as the cure to end all ills, a miraculous lifeline thrown to desperate sufferers of diseases for which conventional medicine offers no hope.
Heart disease, Parkinson’s, multiple sclerosis, diabetes, stroke, Alzheimer’s, muscular dystrophy, spinal injuries and more – believe those who peddle miracle cures, and there is no dead or damaged part of the human body that cannot be regenerated by stem cells.
It is easy to understand why someone facing their own terminal decline or a loved one’s would try anything and spend any amount of money to save their lives.
But mainstream medical practitioners say they are being sold more hype than hope. After all, if there really was a cure for any of these diseases, it would have been marketed by the global pharmaceutical industry long ago.
True, research is continuing around the world into possible benefits of stem cell treatments, as it has for decades. A search of Pubmed, the US National Library’s online repository of global biomedical research, shows that in the past year more than 11,000 papers have been published on the subject.
None of it, says the International Society for Stem Cell Research (ISSCR), has so far altered one stubborn fact: “The list of diseases for which stem cell treatments have been shown to be beneficial is still very short.”
The best-known stem cell treatments are bone marrow or cord blood transplants, used successfully for many years to treat blood and immune system disorders including leukaemia, lymphoma and sickle cell anaemia. Stem cells also play a supporting role in some bone and skin grafts.
But “all other applications of stem cells are yet to be proven in clinical trials and should be considered highly experimental”.
That’s why a joint announcement from the UCL Institute of Ophthalmology and Moorfields Eye Hospital in London has sent ripples of excitement through the global medical research community.
Wet age-related macular degeneration (AMD) is the leading cause of sight loss in the developed world. The macula, the central part of the retina at the back of eye, begins to deteriorate and central vision becomes increasingly blurred. Reading becomes difficult, then impossible. Faces become indistinct.
There was no cure. Until now, possibly.
In September, the first of 10 carefully selected patients underwent a pioneering new treatment that has been a decade in development.
A patch of specialist eye cells, grown in a lab from blank-slate “pluripotent” stem cells harvested from discarded embryos in an IVF programme, and chemically “trained” to evolve into macula tissue, was inserted into the patient’s eye during a two-hour operation.
The identity of the patient is not being revealed but, says Moorfields, “the team hopes to determine her outcome in terms of initial visual recovery by early December”.
If the operation works, that would be a great Christmas present.
During the next 18 months, proceeding cautiously, one operation and the necessary recovery and monitoring period at a time, nine more patients will be treated.
There is no point besieging the hospital in the hope of getting on the programme. Although “we hope that many patients may benefit in the future”, says Prof Pete Coffey of the UCL Institute of Ophthalmology, the trial “focuses on a small group of AMD patients who have experienced sudden severe visual loss”.
Retinal surgeon Prof Lyndon da Cruz from Moorfields Hospital, which has a branch clinic in Dubai, believes the trial will have huge significance for the future of stem cell therapy throughout medicine.
“It’s exciting because we feel we’ve delivered the real deal that was promised for stem cells,” he said.
“Not the outcome, yet, but this is the type of project for which stem cells could be extraordinarily revolutionary: to take a stem cell which can become anything and turn it into something that you want that’s useful for the patient and transplanted successfully into that patient in the midst of disease.”
As for the stem cell treatments being marketed around the world to patients with a wide range of diseases, “most are to fill the void for people with untreatable conditions who are desperate”.
The UCL-Moorfields team has “taken within a very tight UK regulatory framework a stem cell that is truly undifferentiated, that could become anything, and we have driven it to become a very specific layer of the retina.
“We have also demonstrated to the regulator that we are able to make recurrently and safely a perfect copy of a part of the retina.”
That, he says, may be a sufficient demonstration of the promise of stem cell even if they were dealing with a rare condition.
But AMD is the most common cause of vision loss in the western world “and so this achievement is doubly useful. One, it’s proof of principle about the stem cell promise, and two, if it all goes the way we would like it will have a big impact”.
Roger Barker, professor of clinical neuroscience and honourary consultant in neurology at the University of Cambridge and at Addenbrooke’s Hospital, has been working on the application of stem cell therapy in the treatment of Parkinson’s disease for 25 years.
Stem cells, Prof Barker says, undoubtedly hold “enormous potential. In theory, a stem cell source could be used to replace any injured organ or population of cells that are affected by disease”.
But such a breakthrough is “not around the corner. The problem is that simply turning a cell into, say, a heart muscle, is one thing, but making sure it’s properly connected to the electrical system of the heart so it actually functions as it should do is a critical question”.
In his own field, he and other researchers are working towards recreating the damaged specialised brain cells that cause Parkinson’s. “We now have a protocol where we think we can take embryonic stem cells and turn them into dopamine cells. The next big step will be doing all of that to a clinical grade, testing them for safety in preclinical animal models and then negotiating the regulatory process to take that to a first in human trial.”
That, Prof Barker thinks, could take another two or three years, which explains his irritation when he hears of clinics offering stem cell treatments for Parkinson’s.
“I feel sorry for the patients,” he says. “We get a lot of emails from people saying they’ve found this clinic and asking if they should go and have this therapy.
“When you have a disease for which there is no cure then obviously you are looking for anything, but these clinics prey on people’s desperation and are exploiting them financially.”
There are many of these clinics advertising on the internet, especially in the US and China, offering treatments and testimonials from the thousands of patients they claim to have treated successfully.
Three such companies are Stem Cells Egypt, Stem Cells Arabia and Stem Cells Middle East, all of which target the lucrative Middle East market – and all of them appear to be the businesses of one man.
Dr A A Hakim, a urologist based in Minnesota whose CV says he trained at the University of Alexandria in Egypt, claims to operate in conjunction with a Chinese company, Beike Biotechnology, offering stem cell treatments in China and Thailand.
His websites hold hope of cures for conditions including Parkinson’s disease, autism, congestive heart failure and multiple sclerosis.
The UK’s Multiple Sclerosis Society is not so confident. It funds a range of research into the potential of stem cells and says that while they have “the potential to help treat many different conditions”, work is still under way “to try to understand how these cells could be applied to the treatment of MS”.
Dr Hakim, who claims to have treated 15,000 patients with stem cells, declined to discuss what procedure he used to administer them, what qualified him to offer the therapy, what published research he had carried out in the field and how much he charged patients.
He also declined to supply evidence to back his claim that “stem cell treatment is the only effective treatment for 13 chronic diseases”, including diabetes, MS, spinal cord injury, autism and Parkinson’s disease – a claim that appears to fly in the face of accepted medical wisdom.
For now, the advice of the experts is “buyer beware” – no matter how desperate your condition.
EuroStemCell, a partnership of more than 400 European labs and research centres set up “to help European citizens make sense of stem cells”, says that although scientists are investigating the possibility of using stem cells to treat a range of conditions and there is “hope beyond the hype”, it is “still too early to know whether any of these applications will work.
“We need the evidence gathered through a clinical trial process to determine whether a proposed treatment is safe and effective.”
In the meantime, says the ISSCR, “beware of stem cell treatments offered without regulatory approval or outside the confines of a legitimate and registered clinical trial. Unproven treatments present serious health, personal and financial considerations.”
newsdesk@thenational.ae